Insurance credentialing is no longer just an administrative requirement; it is a core driver of revenue cycle performance in 2026. With increasing payer scrutiny, stricter compliance checks, and automated verification systems, delays in credentialing can significantly slow down reimbursement and patient access.
Industry data shows that credentialing delays can extend time-to-first-bill by 90–180 days, resulting in delayed reimbursement, increased accounts receivable (AR) days, and a higher risk of claim denials, payment holds, or suspended reimbursements.
This guide breaks down how credentialing impacts revenue, what causes delays, and how healthcare practices can streamline the process to start billing faster without compromising compliance.
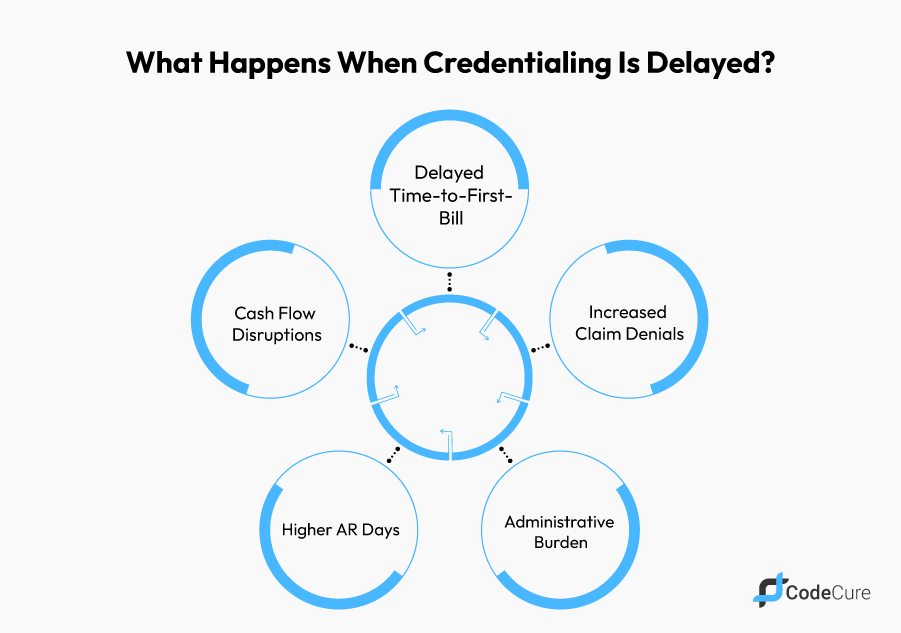
Why Insurance Credentialing Is a Revenue-Critical Process
Insurance credentialing is often misunderstood as a back-office administrative task, but in reality, it is one of the most important drivers of revenue cycle performance. It determines when a provider can legally bill, how quickly claims get reimbursed, and how smoothly a practice can operate financially.
In today’s payer-driven healthcare environment, credentialing directly impacts revenue generation, patient access, claim acceptance rates, and overall financial stability. Any delay in this process creates a ripple effect across scheduling, billing, and collections.
Below are the key reasons credentialing is a critical revenue function rather than just an administrative requirement.
- Faster Patient Access and Revenue Activation
Credentialing is the gateway to patient care reimbursement. Only fully credentialed and enrolled providers can see insured patients under payer contracts and submit reimbursable claims.
When credentialing is delayed, providers are often forced to:
- Delay patient onboarding under insurance plans
- Provide out-of-network or self-pay services
- Postpone billable services entirely
This directly impacts revenue activation timelines and slows down practice growth. Faster credentialing means faster appointment scheduling, quicker patient flow, and immediate billing capability, helping practices generate revenue sooner rather than later.
- Improved Claim Acceptance and First-Pass Resolution Rates
Accurate credentialing ensures that provider information is correctly loaded into payer systems, which directly affects claim acceptance.
When credentialing is incomplete or inconsistent, claims are more likely to face:
- Rejections due to the provider not being found in the payer system
- Denials related to enrollment or taxonomy mismatches
- Delays caused by eligibility verification failures
Proper credentialing significantly improves first-pass claim acceptance rates, reduces administrative rework, and minimizes costly resubmissions. This leads to cleaner claims, faster adjudication, and improved billing efficiency across the revenue cycle.
- Stronger Revenue Cycle Performance and Reduced AR Days
Credentialing delays have a direct impact on Accounts Receivable (AR) performance. When providers are not fully credentialed, claims cannot be submitted or are held in suspense, leading to:
- Increased AR aging buckets
- Delayed reimbursement cycles
- Unpredictable cash flow patterns
- Higher administrative workload in follow-ups and corrections
A streamlined credentialing process shortens time-to-first-bill and helps maintain consistent cash inflow. This stability is essential for both small practices and large healthcare organizations aiming to optimize revenue cycle management (RCM) performance.
- Compliance Readiness and Audit Risk Reduction
Credentialing is also a compliance safeguard that ensures providers meet payer, state, and federal requirements before billing insurance plans.
Proper credentialing helps maintain:
- Up-to-date provider enrollment records
- Accurate NPI, taxonomy, and licensing data
- Verified malpractice insurance and certifications
- Alignment with CMS and payer-specific guidelines
Failure to maintain accurate credentialing records can lead to claim recoupments, audits, or even termination from payer networks. Strong credentialing practices reduce regulatory exposure while ensuring ongoing billing eligibility.
- Operational Efficiency and Reduced Administrative Burden
Beyond revenue impact, credentialing also plays a major role in operational efficiency. Poorly managed credentialing processes often lead to constant follow-ups, missing documentation, and repeated payer communication.
A well-structured credentialing system:
- Eliminates duplicate work
- Reduces staff workload in billing and enrollment teams
- Improves coordination between clinical and administrative departments
- Enhances visibility into provider status across payers
This allows staff to focus on higher-value revenue cycle tasks such as denial management and payment optimization.
- Competitive Advantage in Patient Acquisition
In many specialties, credentialing speed directly affects market competitiveness. Practices that complete credentialing faster can:
- Onboard providers sooner
- Expand insurance participation faster
- Capture more insured patient volume
- Increase referral acceptance rates
Delays in credentialing not only slow revenue but also limit a practice’s ability to compete in insurance-driven markets where network participation is a key factor in patient decision-making.
Insurance credentialing is not a standalone administrative function it is a foundational revenue cycle process that influences billing speed, claim accuracy, compliance readiness, and overall financial performance. Practices that treat credentialing as a strategic RCM priority consistently experience:
- Faster revenue activation
- Higher claim acceptance rates
- Lower AR days
- Stronger compliance protection
- Improved operational efficiency
Common Causes of Credentialing Delays
Even highly organized healthcare practices experience bottlenecks in insurance credentialing. These delays are usually not caused by a single issue, but by a combination of documentation gaps, payer workflows, and process inefficiencies. Understanding these root causes is essential to reducing turnaround time and improving revenue cycle performance.
- Incomplete or Inaccurate Applications
One of the most frequent causes of credentialing delays is incomplete or incorrect application submission. Missing licenses, unsigned forms, outdated malpractice insurance, or inconsistent provider details can immediately place an application on hold.
Even minor discrepancies such as mismatched addresses, incorrect taxonomy codes, or missing attachments can trigger payer rejections or reprocessing requests. This often adds several weeks or even months to the overall credentialing timeline.
- Slow and Manual Payer Verification Processes
Insurance payers are required to independently verify provider credentials, including medical licenses, board certifications, DEA registration, and malpractice coverage. However, many payers still rely on manual or semi-automated verification systems.
This dependency on manual review creates unavoidable delays, especially when payer backlogs are high or when additional verification is required with licensing boards or external databases. As a result, even complete applications can remain pending for extended periods.
- Missing, Outdated, or Inconsistent Provider Data
Provider data accuracy plays a critical role in credentialing success. Applications are often delayed when key information is missing or outdated, such as:
- Expired DEA registration or state license
- Incorrect National Provider Identifier (NPI) details
- Gaps in employment history or practice affiliations
- Inconsistent information across CAQH, PECOS, and payer portals
These inconsistencies often trigger additional verification steps, slowing down approval and increasing administrative workload.
- Lack of Standardized Credentialing Workflow Across Payers
Each insurance payer follows different credentialing requirements, documentation formats, and submission protocols. Without a standardized internal process, practices often submit applications inconsistently across payers.
This lack of standardization leads to:
- Repeated document requests
- Submission rework
- Delays due to missing payer-specific forms
- Inefficient communication between staff and payers
A structured, uniform submission process is essential to avoid unnecessary back-and-forth delays.
- Absence of Centralized Tracking and Follow-Up System
Without a dedicated credentialing tracking system, applications can easily become unmonitored after submission. This leads to missed follow-ups, delayed responses to payer requests, and lack of visibility into application status.
In many practices, credentialing tasks are scattered across emails, spreadsheets, and individual staff members, creating gaps in accountability. A centralized tracking system ensures timely follow-ups, better organization, and significantly reduced processing time.
Credentialing delays are rarely caused by a single factor. Instead, they stem from a combination of incomplete documentation, manual payer workflows, inconsistent data management, and lack of structured tracking systems. Addressing these core issues helps healthcare practices significantly reduce credentialing timelines, improve payer responsiveness, and accelerate time-to-first-bill.
Step-by-Step Guide to Speed Up Insurance Credentialing in 2026
A structured and proactive credentialing workflow can significantly reduce approval timelines, improve payer responsiveness, and accelerate time-to-first-bill. In 2026, practices that rely on manual or reactive processes often experience longer delays, while those using standardized and technology-driven approaches achieve faster enrollment and stronger revenue cycle performance.
Below is a practical step-by-step framework to streamline insurance credentialing.
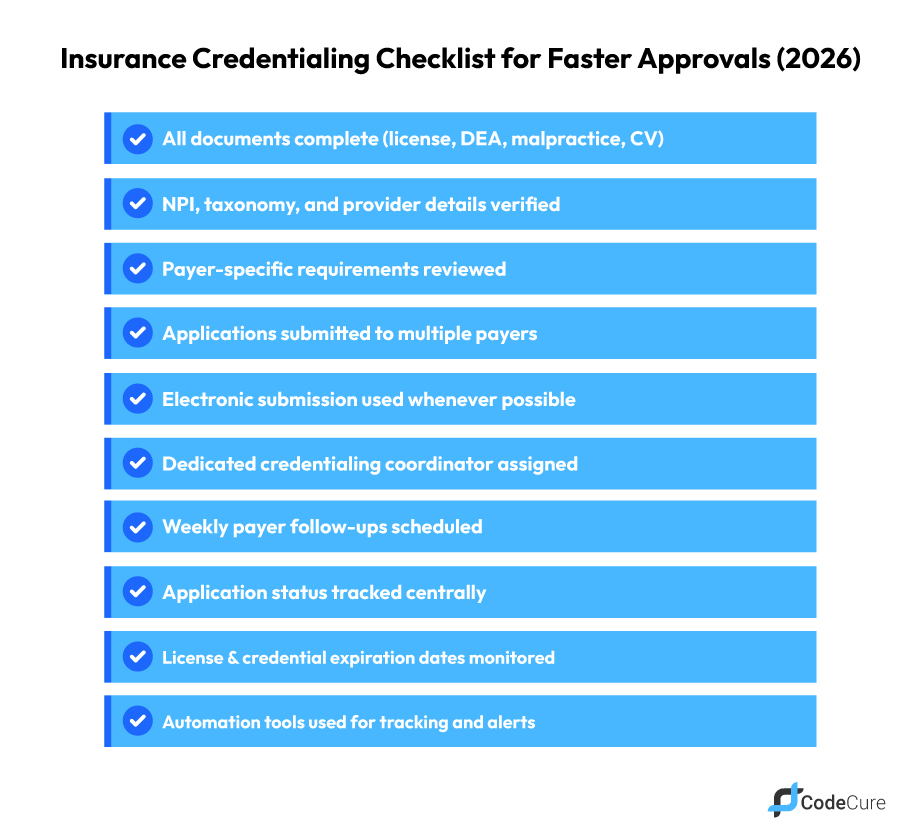
1. Prepare a Complete Credentialing Package in Advance
One of the most effective ways to reduce delays is to ensure all provider documentation is complete, verified, and updated before submission.
This typically includes:
- Active medical license(s)
- DEA registration
- Board certifications
- Malpractice insurance certificate
- Updated CV with accurate employment history
- Hospital affiliations (if applicable)
- NPI details and taxonomy codes
Having a fully prepared credentialing packet minimizes errors, reduces payer follow-up requests, and significantly improves approval speed.
2. Review and Align with Individual Payer Requirements
Each insurance payer follows its own credentialing policies, documentation standards, and submission workflows. Failing to align with these requirements is a common cause of delays and rejections.
Before submitting applications, practices should carefully review:
- Payer-specific credentialing forms
- Submission methods (electronic vs. paper-based)
- Required supporting documentation
- Network participation rules
Tailoring each application to payer expectations ensures smoother processing and fewer rework cycles.
3. Leverage Credentialing Software or Professional Outsourcing
Modern credentialing platforms and RCM service providers play a critical role in improving efficiency and accuracy.
These solutions help by:
- Tracking application status in real time
- Automating follow-ups and reminders
- Validating provider credentials across databases
- Reducing manual administrative workload
Outsourcing credentialing to specialized teams can further reduce turnaround time, improve accuracy, and free internal staff to focus on revenue-generating activities.
4. Assign a Dedicated Credentialing Coordinator
Centralized ownership of the credentialing process is essential for consistency and accountability.
A dedicated credentialing specialist ensures:
- All applications are properly submitted and tracked
- Follow-ups are completed on schedule
- Provider credentials are monitored for expiration
- Communication with payers is streamlined and documented
This eliminates fragmented workflows and reduces the risk of missed applications or delays.
5. Submit Applications to Multiple Payers in Parallel
Submitting credentialing applications sequentially can significantly slow down revenue activation.
A parallel submission strategy applying to multiple payers simultaneously helps:
- Reduce overall credentialing timelines
- Accelerate network participation
- Enable faster billing across multiple insurance plans
This approach is especially important for new practices or newly added providers.
6. Establish a Consistent Follow-Up System
Regular and structured follow-ups are critical to keeping applications moving through payer systems.
Effective follow-up practices include:
- Weekly or bi-weekly status checks
- Immediate response to payer documentation requests
- Proactive clarification of missing or unclear information
Consistent communication reduces stagnation in payer queues and improves overall approval speed.
7. Prepare in Advance for Site Visits and Credentialing Interviews
Some payers may require on-site inspections or provider interviews as part of the credentialing process.
To avoid delays, practices should ensure:
- Compliance documentation is organized and accessible
- Office operations meet payer standards
- Staff are prepared to respond to verification questions
- Policies and procedures are clearly documented
Proper preparation ensures these final steps do not become approval bottlenecks.
8. Implement Digital Credentialing Systems and EHR Integration
Modern healthcare organizations increasingly rely on digital infrastructure to streamline credentialing workflows.
Integrated EHR and RCM systems support:
- Automated tracking of license and certification expirations
- Real-time credentialing status monitoring
- Alerts for pending tasks or missing documentation
- Seamless integration between credentialing and billing workflows
Digital transformation reduces manual errors, improves compliance visibility, and significantly shortens credentialing cycles.
Speeding up insurance credentialing in 2026 requires a combination of preparation, standardization, automation, and proactive management. Practices that implement structured workflows and digital tools consistently experience faster payer approvals, improved revenue cycle efficiency, and reduced time-to-first-bill.
Common Credentialing Mistakes to Avoid
Even well-managed healthcare practices can experience significant delays in insurance credentialing due to avoidable process gaps. These mistakes not only slow down approvals but also directly impact revenue cycle performance, claim readiness, and time-to-first-bill.
Understanding and preventing these issues is essential for faster payer enrollment and smoother billing operations.
- Submitting Incomplete or Inaccurate Applications
One of the most common causes of credentialing delays is submitting applications with missing, outdated, or inconsistent information.
This includes:
- Expired licenses or certifications
- Missing signatures or supporting documents
- Incorrect demographic or provider data
- Inconsistent information across payer systems
Even minor discrepancies can trigger application holds, rejections, or extended verification cycles, significantly delaying approval timelines.
- Processing One Payer at a Time Instead of Parallel Enrollment
Many practices still follow a sequential credentialing approach, submitting applications to one payer at a time. This outdated method unnecessarily prolongs the onboarding process.
In contrast, parallel enrollment across multiple payers allows practices to:
- Reduce overall credentialing timelines
- Accelerate revenue activation
- Improve network participation speed
Failing to adopt a multi-payer strategy often results in delayed billing and slower cash flow generation.
- Overlooking Payer-Specific Credentialing Requirements
Each insurance payer has its own credentialing criteria, documentation formats, and submission workflows. Ignoring these differences is a major source of rework and delays.
Common issues include:
- Submitting incorrect or outdated forms
- Missing payer-specific attachments
- Not following electronic submission protocols
Failure to align with payer expectations often leads to repeated correction requests and extended processing times.
- Lack of Dedicated Credentialing Ownership
Credentialing processes require consistent monitoring, follow-ups, and coordination across multiple stakeholders. Without a dedicated credentialing coordinator or team member, applications often become fragmented or neglected.
This leads to:
- Missed follow-ups with payers
- Delayed responses to documentation requests
- Lack of visibility into application status
- Increased risk of lost or stalled applications
Centralized ownership is critical for maintaining workflow continuity and accountability.
- Failure to Monitor Credential Expiration and Revalidation Dates
Expired credentials are a hidden but significant cause of billing interruptions. When licenses, certifications, or insurance coverage lapse, providers may become temporarily ineligible for reimbursement.
Common oversights include:
- Expired medical or state licenses
- Lapsed DEA registrations
- Outdated malpractice insurance coverage
- Missed payer revalidation deadlines
Without proactive tracking, these issues can lead to claim denials, payment holds, or temporary network termination.
- Dependence on Manual and Paper-Based Credentialing Processes
Manual credentialing workflows significantly increase the risk of human error and processing delays. Paper-based tracking systems, spreadsheets, and email-only communication often lack structure and accountability.
This results in:
- Lost or misfiled documents
- Missed deadlines and follow-ups
- Limited visibility into application status
- Slower overall approval cycles
Modern credentialing requires digital tracking systems and automated workflows to ensure accuracy, speed, and compliance.
Avoiding these common credentialing mistakes is essential for reducing administrative delays and improving revenue cycle performance. Practices that implement standardized workflows, digital tracking systems, and centralized ownership consistently achieve faster payer approvals, fewer denials, and improved financial outcomes.
How to Sustain Faster Credentialing Long-Term
Maintaining fast and efficient credentialing requires ongoing structure and consistency. Without proper systems in place, delays can return due to missed renewals, data errors, or process gaps.
- Maintain a Credentialing Calendar
Track all key dates such as license renewals, payer revalidations, and certifications to prevent lapses and billing interruptions.
- Standardize Submission Templates
Use consistent credentialing forms and workflows across all payers to reduce errors and rework.
- Audit Provider Files Regularly
Review provider data, licenses, and payer profiles to ensure accuracy and avoid discrepancies.
- Use Automation Tools
Leverage credentialing software to track expirations, send alerts, and monitor application status.
- Conduct Quarterly Reviews
Evaluate turnaround times, delays, and workflow issues to continuously improve the process.
Sustaining fast credentialing depends on consistency, automation, and regular monitoring. Practices that follow structured processes maintain faster approvals and stronger revenue cycle performance over time.
Accelerate Credentialing with CodeCure
CodeCure streamlines insurance credentialing from start to finish so healthcare practices can get providers enrolled faster, reduce payer delays, and start billing without long waiting periods. From documentation and payer submissions to real-time tracking, follow-ups, and credential maintenance, we manage the entire process with an RCM-focused, automated approach that eliminates bottlenecks and improves revenue readiness. Instead of waiting months for approvals, your practice can accelerate enrollment, reduce administrative burden, and keep cash flow moving from day one.
Conclusion
Insurance credentialing is no longer just a backend administrative task; it is a core revenue cycle function that directly impacts cash flow, claim acceptance, and practice growth. In 2026, practices that rely on manual processes continue to face unnecessary delays, while those using structured, automated credentialing systems achieve faster payer approvals and stronger financial stability.
If your practice is struggling with credentialing delays or slow payer enrollment, CodeCure can help you streamline the entire process and get your providers billing faster.
Partner with CodeCure today to simplify credentialing, improve revenue cycle efficiency, and ensure faster reimbursement in 2026.
Frequently Asked Questions (FAQ)
- What is insurance credentialing?
Insurance credentialing is the process of verifying a healthcare provider’s qualifications and enrolling them with insurance payers so they can legally bill for services and receive reimbursements.
- How long does credentialing take in 2026?
On average, credentialing takes 60–180 days, depending on the payer, specialty, and how complete the application is. Delays often extend timelines when documentation or follow-ups are missing.
- Why does insurance credentialing take so long?
Delays usually occur due to incomplete applications, slow payer verification processes, missing provider information, and a lack of consistent follow-ups or tracking systems.
- Can credentialing be expedited?
Yes. Credentialing can be significantly sped up by submitting complete applications, applying to multiple payers simultaneously, using automation tools, and maintaining proactive follow-ups.
- What documents are required for credentialing?
Common documents include a medical license, DEA registration, board certifications, malpractice insurance, CV, hospital affiliations, and accurate NPI and taxonomy details.
- What happens if a provider is not credentialed?
If a provider is not credentialed, they cannot bill insurance payers, which leads to delayed revenue, denied claims, or patients being treated as self-pay or out-of-network.
- How does CodeCure help with credentialing?
CodeCure manages the full credentialing process, including documentation, payer enrollment, tracking, follow-ups, and credential maintenance to help practices reduce delays and start billing faster.





