In today’s fast-paced healthcare environment, ensuring that your cardiology practice stays compliant, efficient, and fully reimbursed is more critical than ever. One of the most important steps in achieving this is credentialing, specifically, cardiology credentialing, which has its unique challenges and requirements. At CodeCure, we understand that navigating the credentialing and enrollment process can be a daunting task for cardiologists. This blog will guide you through the essential steps of cardiology credentialing, why it matters, and how to streamline this process for faster approvals and fewer denials.
What is Cardiology Credentialing and Why is It Important?
Credentialing is the process of verifying that healthcare providers meet all the necessary qualifications to provide services to patients and receive reimbursement from insurance companies. In cardiology, this process is more complex due to the specialized nature of the services provided.
Cardiologists must meet strict guidelines to get credentialed with Medicare, Medicaid, and various commercial insurance carriers. This ensures that your practice is not only compliant with federal and state regulations but also able to maximize reimbursements and avoid payment delays. If this process is not handled correctly, it can lead to costly denials, compliance issues, and, most importantly, disruption in patient care.
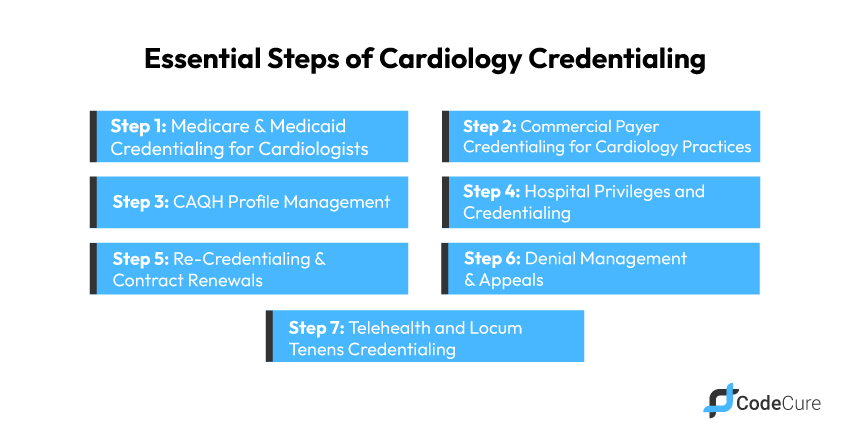
Step 1: Medicare & Medicaid Credentialing for Cardiologists
Medicare and Medicaid are the two largest payers for cardiology services. Whether you’re a solo cardiologist or part of a multi-provider practice, getting approved for these programs is crucial.
What’s involved in the process?
- Medicare Enrollment: Cardiologists must complete a PECOS (Provider Enrollment, Chain, and Ownership System) application and meet certain state-specific Medicaid requirements. Without approval, your ability to bill Medicare for services is jeopardized.
- Medicaid Enrollment: State Medicaid programs each have their own criteria, but at CodeCure, we ensure all necessary paperwork is completed and submitted accurately to avoid unnecessary delays.
Why is this step so important? A smooth and quick Medicare/Medicaid credentialing process ensures that you receive the proper reimbursements for services, keeping your practice financially stable and compliant.
Step 2: Commercial Payer Credentialing for Cardiology Practices
Beyond government programs, cardiology practices also need to get credentialed with commercial payers like Aetna, Blue Cross Blue Shield (BCBS), Cigna, and UnitedHealthcare. While these insurers often have different requirements, they all require up-to-date documentation, including:
- Board certifications
- DEA licenses
- Hospital affiliations
What’s the Process?
- Payer Enrollment: Commercial insurers require a series of forms and background checks, ensuring that your practice is in good standing before they allow you to bill for cardiology services.
- Contract Compliance: Each payer has its own set of rules and contract terms. Our team at CodeCure helps ensure you stay on top of contract renewals and compliance requirements, preventing unnecessary delays.
Why Is This Important? Proper enrollment with commercial insurers allows you to build relationships with top payers, ensuring you’re reimbursed for the full range of services you provide, from routine cardiology visits to complex procedures like catheterizations or device implantations.
Step 3: CAQH Profile Management – The Key to Streamlined Enrollment
The Council for Affordable Quality Healthcare (CAQH) ProView is a critical system used by insurers to verify provider credentials. Managing this profile effectively can significantly reduce the time it takes to get credentialed with multiple insurers.
What’s involved in CAQH Profile Management?
- Updating Information: Ensure your CAQH profile is current with accurate details about your practice, including education, training, and certifications.
- Automated Reminders: We help set up automated reminders for updating your profile to avoid missing deadlines.
Why Is This Important? A properly managed CAQH profile is essential for reducing redundant paperwork, avoiding errors, and speeding up the approval process with insurers, thus preventing potential payment delays or denials.
Step 4: Hospital Privileges and Credentialing
Many cardiologists work with hospitals or heart centers to provide specialized procedures. In these cases, hospital privileges are required, meaning you must be credentialed by the hospital itself.
What’s involved in hospital credentialing?
- Privileges Applications: Hospitals require cardiologists to submit an application and verify their background and certifications.
- Re-credentialing: Credentialing isn’t a one-time event. Re-credentialing occurs at regular intervals, often every two years, to ensure continued eligibility.
Why Is This Important? Hospital credentialing ensures you have the necessary privileges to perform life-saving procedures like catheterizations or stent placements. It protects your ability to provide high-quality care and receive reimbursement for these services.
Step 5: Re-Credentialing & Contract Renewals – Keeping Your Practice Updated
Credentialing is not a one-and-done process. Every few years, providers must go through re-credentialing to maintain their eligibility with payers and hospitals. This ensures that your practice stays compliant and doesn’t experience any lapses in coverage.
What’s involved in re-credentialing?
- Monitoring Deadlines: Staying on top of credentialing and contract renewal deadlines is essential to avoid interruptions in billing and reimbursement.
- Document Updates: As regulations and requirements evolve, it’s important to keep your documentation up to date.
Why Is This Important? Failing to stay current with re-credentialing requirements can lead to lapsed contracts, missed reimbursements, and even compliance penalties.
Step 6: Denial Management & Appeals – Recovering Lost Revenue
Even with all the correct credentials in place, denials can still happen. Credentialing errors, missing documentation, or incorrect coding can all lead to rejected claims. At CodeCure, we help practices manage these denials by:
- Identifying Root Causes: We track and analyze the reasons behind each denial.
- Submitting Appeals: Once the issue is identified, we help submit appeals and follow up with payers to get claims processed and paid.
Why Is This Important? Having a streamlined denial management process ensures that lost revenue is recovered quickly, allowing you to focus on providing excellent patient care without financial disruptions.
Step 7: Telehealth and Locum Tenens Credentialing
The rise of telehealth has transformed the way cardiology care is delivered. Credentialing for telehealth providers or locum tenens staff (temporary or substitute cardiologists) is a unique challenge but critical for ensuring compliance and reimbursement.
What’s involved in telehealth credentialing?
- Credentialing for Virtual Care: We ensure that telehealth providers meet the necessary requirements to bill for virtual consultations, remote monitoring, and other telehealth services.
- Locum Tenens Coverage: Temporary cardiologists also need to be credentialed with all relevant payers, just like full-time providers.
Why Is This Important? Telehealth and locum tenens services can expand your practice’s reach and help meet patient needs without reimbursement risks. Proper credentialing ensures that virtual care and temporary staffing are fully compliant with payer rules.
Cardiology Credentialing Application Checklist
This cardiology credentialing application checklist outlines the exact information and documents required to complete Medicare, Medicaid, CAQH, commercial payer, and hospital applications accurately. It helps cardiology practices avoid incomplete submissions, reduce approval delays, and prevent credentialing-related claim denials.
Practice Information
✔ Legal practice name
✔ DBA (if applicable)
✔ Tax ID (EIN)
✔ NPI Type 2 (Group)
✔ Practice address(es)
✔ Phone, fax, email
✔ W-9 (signed & current)
✔ Ownership disclosure
Provider Application Data
✔ Provider full legal name
✔ NPI Type 1
✔ SSN (for enrollment)
✔ Date of birth
✔ Medical license number(s)
✔ License expiration date(s)
✔ Cardiology specialty & subspecialty
Education & Certification
✔ Medical school details
✔ Residency (Cardiology/Internal Medicine)
✔ Fellowship (Interventional, EP, HF, Imaging, etc.)
✔ Board certification / eligibility
✔ Certification expiration date
DEA & Prescribing
✔ DEA number
✔ DEA expiration date
✔ State CDS (if required)
Professional History
✔ Work history (last 5–10 years)
✔ Explanation of gaps (if any)
✔ Hospital affiliations
Malpractice Insurance
✔ Carrier name
✔ Policy number
✔ Coverage limits
✔ Effective & expiration dates
✔ Claims history (if applicable)
Medicare Application (PECOS)
✔ CMS-855B (group)
✔ CMS-855I (individual)
✔ CMS-855R (reassignment)
✔ Practice location linked
✔ EFT & ERA forms
Medicaid Application
✔ State Medicaid application
✔ Provider linkage to group
✔ Managed Medicaid plans selected
✔ EFT enrollment
Commercial Payer Applications
✔ CAQH ProView ID
✔ CAQH authorization granted
✔ Payer-specific forms completed
✔ Contracts acknowledged
Hospital / Facility Privileges
✔ Privileging application
✔ Procedure list (Cath lab, EP lab, etc.)
✔ References submitted
Telehealth / Locum (If Applicable)
✔ Telehealth services disclosure
✔ State licensure compliance
✔ Locum tenens documentation
Compliance Attestations
✔ NPDB self-query
✔ OIG exclusion attestation
✔ GSA/SAM check
✔ HIPAA compliance attestation
Final Application Review
✔ All fields completed
✔ Dates consistent across forms
✔ Documents uploaded
✔ Signatures applied
✔ Submission confirmation saved
Tips for Cardiology Practices
- Always submit applications only after licenses, DEA, and malpractice are active to avoid automatic rejections.
• Ensure dates, addresses, and provider details match across CAQH, PECOS, and payer forms to prevent delays.
• Track re-credentialing and contract renewal deadlines proactively to avoid payment interruptions.
How CodeCure Can Help Your Practice Streamline Credentialing & Enrollment
At CodeCure, we specialize in making the credentialing and enrollment process seamless for cardiology practices. Here’s how we can help you:
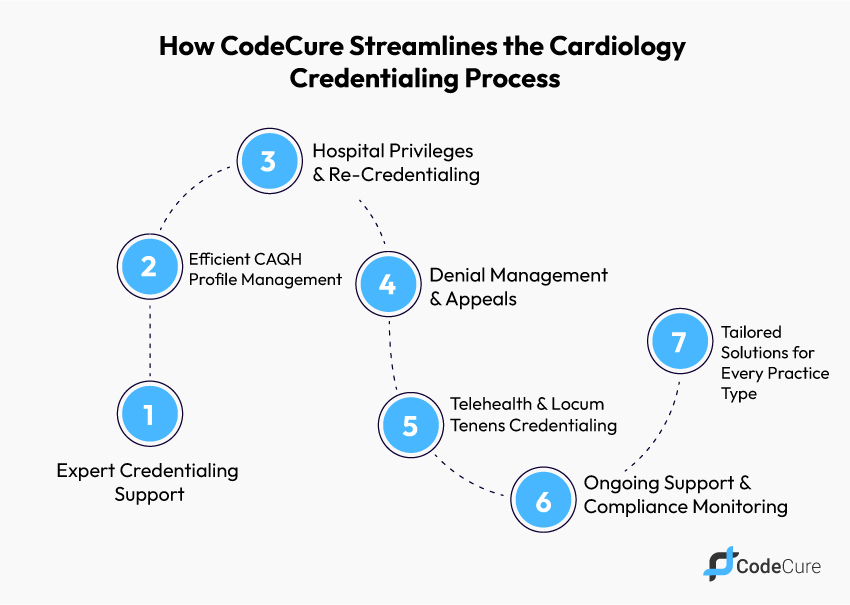
- Expert Credentialing Support
We understand that cardiology credentialing is more complex than standard medical credentialing. Our team of experts manages the entire process, from Medicare/Medicaid enrollment to commercial payer credentialing and hospital privileges. We ensure that every detail is handled accurately and efficiently, helping your practice stay compliant and avoid costly delays.
- Efficient CAQH Profile Management
Managing your CAQH profile can be time-consuming and tedious. CodeCure optimizes your profile with accurate updates and automated reminders, ensuring that your credentials are always up to date for smoother and faster payer approvals.
- Hospital Privileges & Re-Credentialing
Whether you need to apply for hospital privileges or manage re-credentialing, CodeCure ensures that your documentation is complete and compliant, preventing interruptions in your ability to provide critical care to your patients.
- Denial Management & Appeals
If you face denials due to credentialing errors, our team will help identify the root causes, provide corrected documentation, and submit timely appeals. We’ll ensure that lost revenue is recovered and avoid repeated payer rejections.
- Telehealth & Locum Tenens Credentialing
CodeCure ensures that your telehealth providers and locum tenens cardiologists meet all the necessary credentialing requirements for virtual care and temporary staffing, helping you expand your practice without worrying about compliance issues.
- Ongoing Support & Compliance Monitoring
We provide continuous monitoring of credentialing deadlines, ensuring that your practice stays compliant with ever-evolving regulations. With CodeCure, you’ll never have to worry about missing a credentialing deadline or falling out of compliance.
- Tailored Solutions for Every Practice Type
Whether you’re a solo cardiologist, part of a multi-provider clinic, or managing a heart center, we offer tailored credentialing solutions that fit your unique needs. CodeCure ensures that your practice can focus on what truly matters: patient care.
Conclusion:
Credentialing can be a complex, time-consuming process, but it doesn’t have to be overwhelming. By partnering with CodeCure, you can ensure your cardiology practice stays compliant, avoids costly delays, and maximizes reimbursements. Our expert team handles every step of the credentialing and enrollment process, allowing you to focus on what truly matters to your patients.
If you’re ready to streamline your credentialing and enrollment processes, avoid denials, and stay fully compliant with payer requirements, reach out to CodeCure today. We’re here to support you every step of the way!
FAQS:
What is cardiology credentialing and why is it important?
Cardiology credentialing is the process of verifying a cardiologist’s qualifications to provide services and receive reimbursements from insurance companies. It is essential for compliance with regulations, ensuring timely reimbursements, and avoiding costly denials or payment delays.
How long does the cardiology credentialing process take?
The credentialing process typically takes between 30 to 90 days, depending on the complexity and the payer. It can be faster if all required documentation is complete and submitted correctly.
How can CodeCure help with cardiology credentialing?
CodeCure offers expert support throughout the credentialing process, including Medicare/Medicaid enrollment, commercial payer credentialing, hospital privileges, CAQH profile management, denial management, and more. Our team ensures that your practice stays compliant and avoids costly delays.
What documents are needed for cardiology credentialing?
Commonly required documents include board certifications, DEA licenses, medical school transcripts, malpractice insurance, hospital affiliations, and a completed CAQH profile. Additional documents may be required depending on the payer.
How do I enroll my cardiology practice with Medicare and Medicaid?
To enroll with Medicare and Medicaid, cardiologists must complete a PECOS (Provider Enrollment, Chain, and Ownership System) application for Medicare and meet state-specific Medicaid requirements. CodeCure can assist in completing and submitting these applications to avoid delays.
What is the CAQH profile and how does it help with credentialing?
The CAQH (Council for Affordable Quality Healthcare) ProView profile is a central database used by insurers to verify a provider’s credentials. Properly managing and updating your CAQH profile ensures faster and more efficient enrollment with multiple payers.
What is the difference between credentialing and privileging?
Credentialing verifies that a provider meets the necessary qualifications to offer care, while privileging grants specific rights to perform particular procedures within a hospital or healthcare facility. Both are necessary for cardiologists to provide and get reimbursed for specialized services.
What happens if my cardiology credentialing is delayed?
Delayed credentialing can lead to missed reimbursements, lapsed contracts, and interruptions in patient care. At CodeCure, we streamline the process to minimize delays and ensure that your practice remains compliant and financially stable.
Why is re-credentialing necessary for cardiology practices?
Re-credentialing ensures that your provider information remains up-to-date with insurance companies and hospitals. It is a periodic requirement, typically every 1-3 years, and failure to renew can result in lapses in coverage and disruptions in reimbursements.
How does telehealth credentialing work for cardiology practices?
Telehealth credentialing involves ensuring that providers are credentialed to offer virtual consultations and remote care. It requires meeting the same requirements as in-person care but also includes specific guidelines for telehealth services, including licensure across state lines and telehealth platform compliance.
How do I handle denial management and appeals in cardiology?
Denial management involves identifying the root causes of denied claims, correcting the issues, and submitting appeals to insurance companies. CodeCure helps practices recover lost revenue by managing denials effectively and submitting timely appeals for faster reimbursement.
What are the benefits of outsourcing cardiology credentialing to CodeCure?
Outsourcing to CodeCure saves time and reduces administrative burden. We ensure that all credentialing paperwork is accurate and submitted on time, which leads to faster approvals, fewer denials, and improved cash flow for your practice.
How can CodeCure assist with commercial payer credentialing?
CodeCure works with major insurance carriers like Aetna, BCBS, Cigna, and UnitedHealthcare, helping practices complete payer-specific forms, meet contract terms, and ensure compliance. We handle enrollment, renewals, and document updates to ensure a smooth process.
What is the process for obtaining hospital privileges for cardiologists?
To obtain hospital privileges, cardiologists must submit an application to the hospital, undergo background checks, and provide necessary documentation like certifications and training. CodeCure helps manage this process and ensures timely re-credentialing to avoid interruptions in care.
Can CodeCure help my practice stay compliant with changing regulations?
Yes! CodeCure continuously monitors credentialing and enrollment regulations, ensuring that your practice remains compliant with Medicare, Medicaid, HIPAA, and other regulatory standards. We handle updates and renewals, so you never miss a deadline.






